For babies, sucking is a survival reflex essential for feeding, nourishment and self-regulation. Mouthing or chewing items is part of typical development and Occupational Therapist Claire Joyce describes it as baby’s first sensory learning experience.
Mouthing behaviours typically reduce from the age of 18 months to two years as the central nervous system works more efficiently and development continues upwards through the Pyramid of Learning.
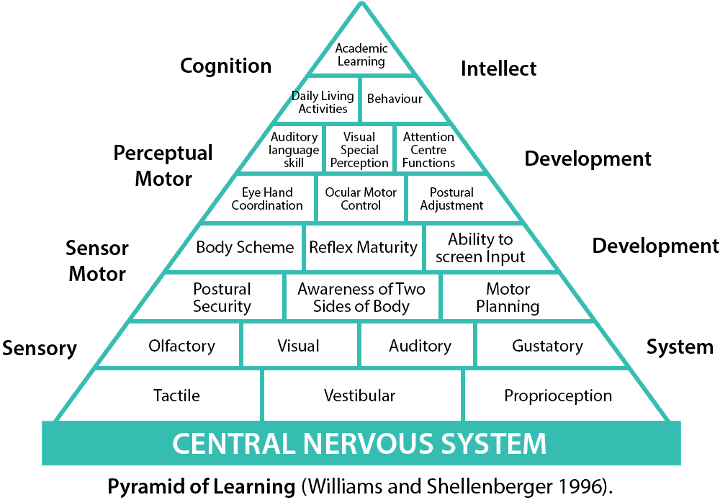
Source: https://kids-first.com.au/how-your-childs-sensory-system-sets-them-up-for-life/
When oral sensory-seeking behaviours continue beyond the age of two years, you may notice sucking or chewing on clothing, toys, thumbs, and fingernails. Possible causes include:
- Developmental delays: Children with developmental delays or sensory processing disorders may seek oral stimulation as a way to regulate their sensory input.
- Anxiety or stress: Children who are anxious or stressed may seek oral stimulation as a way to soothe themselves.
- ADHD or hyperactivity: Children with ADHD or hyperactivity may seek oral stimulation as a way to channel their excess energy.
- Nutritional deficiencies: Children who are deficient in certain nutrients, such as iron or zinc, may seek oral stimulation as a way to satisfy their body's needs.
- Autism: Autistic children may engage in oral sensory seeking behaviour as a way to self-regulate and manage sensory overload.
- Pica: Pica is a condition in which children crave and consume non-food items. Oral sensory seeking may be a symptom of pica.
It's important to note that oral sensory seeking behaviour is not always harmful or problematic.
What are the risks, and how do we minimise them?
Risks associated with children putting non-food items in their mouths include digestive upset and potential choking. In addition, eating sand or dirt may lead to constipation or exposure to parasites, bacteria and heavy metals, and less commonly, intestinal obstruction or perforation.
To minimise these risks, CELA Early Education Specialist Jannelle Gallagher recommends being proactive to understand what is happening for the child. Be informed and consult with parents, other educators, and the child. Read information such as ACECQA's Providing a Child safe Environment, which outlines appropriate supervision, equipment repair and protection from harm and hazards.
Risk assessments for resources used in early childhood settings ensure that equipment offered is safe for all children who may access the space in, considering size, shape, and quantity.
How to respond in the moment
It can be useful to consider your response to these behaviours, suggests Claire, and to reflect on if you want it to stop because it poses a risk or because you feel uncomfortable.
An inclusive approach to play in early childhood settings is recommended, with adaptations made as needed to ensure safety. The child should not be told to stop or moved away unless there is immediate danger to the child's health.
“Moving the child takes away the child’s right to be there,” says Jannelle, who suggests working with the child to clarify why the educator has concerns.
If a child is putting things in their mouth that pose a risk, Jannelle suggests tailored supervision and educator-led play to model safe ways of engaging with the resource or providing resources that allow the child to continue to play in this space in a safe way. Educators can use both verbal and visual cues to assist with this.
How to respond moving forward
Educators can use a scatterplot to look at what’s going on and when it happens, says Jannelle. Open conversations with parents or carers can help us understand more about the contexts in which oral sensory-seeking behaviours occur. If they happen in early education and care settings but not at home, Jannelle suggests looking into whether the behaviours may be anxiety-related.
Ask yourself what is happening for the child at that moment. Has the child built a strong, nurturing relationship with educators?
Educators should approach parents gently when raising developmental concerns. A brief chat in a private setting is best, before referring the family to a health professional. Working in partnership, parents and educators can provide input from their experience. Then, all parties can agree on strategies that respect the child’s right to be included in play.
Gauging where the child is developmentally and responding from a ground-up approach on the Pyramid of Learning helps integrate sensory systems and may reduce oral sensory seeking behaviours over time, says Claire. This may involve activities that promote tactile, proprioceptive, and vestibular development; support from an occupational therapist can guide this.
Learning more about the sensory needs being met by oral sensory seeking helps us explore if they can be met in other ways, such as a chew necklace, cooking experiences exploring textures, playing with textured materials, or tending to an edible garden. There are many tactile receptors in the mouth. Claire suggests introducing edible play resources such as home-made playdough and cooked spaghetti, water play, and messy play, which can help fill a child's “sensory cup”.
.jpg?width=750&height=750) Having a written plan to share with staff and parents outlining safety issues and supervision requirements provides transparency and consistency in communication. Education for children about edible and non-edible items may also be useful, along with a photo book showing the child/children engaging safely with the resources to help consolidate this learning.
Having a written plan to share with staff and parents outlining safety issues and supervision requirements provides transparency and consistency in communication. Education for children about edible and non-edible items may also be useful, along with a photo book showing the child/children engaging safely with the resources to help consolidate this learning.
Understanding why a child engages in oral sensory-seeking behaviours is important for parents and educators. When it comes to these behaviours, the child is learning and exploring through the play they want to engage in, and it is not until this need has been met that the behaviours may begin to decrease.
Conclusion
Mouthing and sucking behaviours are normal and essential for babies' survival and development. However, when these behaviours persist beyond the age of two years, they may indicate underlying issues such as sensory overload, developmental delays, or dental problems. To minimise the risks associated with oral sensory-seeking behaviours, it is essential to maintain a child-safe environment, including well-maintained sandpits, safe equipment, and appropriate supervision. Educators can also respond in the moment by providing tailored supervision and educator-led play to model safe ways of engaging with resources.
Moving forward, open conversations with parents, a ground-up approach to the Pyramid of Learning, and the guidance of occupational therapists can help meet the child's sensory needs and reduce oral sensory-seeking behaviours over time. By understanding the sensory needs of children, educators and parents can introduce alternative ways to meet those needs while ensuring their safety and promoting their inclusion in play.
Sources:
‘Providing a Child Safe Environment – Policy Guidelines’ Australian Children’s Education and Care Quality Authority (ACECQA) https://www.acecqa.gov.au/sites/default/files/2022-03/Providing-a-childsafe-environment-policy.pdf
‘Is It Harmful to Eat Dirt, and Why Do Some People Do It?’ Healthline https://www.healthline.com/health/mental-health/eating-dirt#dangers
‘What is Pica?’ Inside Out Institute https://insideoutinstitute.org.au/resource-library/what-is-pica
‘How Your Child’s Sensory System Sets Them Up for Life’ Kids First https://kids-first.com.au/how-your-childs-sensory-system-sets-them-up-for-life/
‘Staying Healthy: Preventing infectious diseases in early childhood education and care services’ National Health and Medical Research Council – Australian Government, 2013
https://www.nhmrc.gov.au/sites/default/files/documents/attachments/ch55-staying-healthy.pdf
‘What If My Child Eats Kinetic Sand?’ Poison Control – National Capital Poison Center (US)
https://www.poison.org/articles/what-if-my-child-eats-kinetic-sand-204